Predictable Results Through DIEM Guidelines
Richard J. Lazzara, DMD, MScD
Tiziano Testori, MD, DDS
Alan Meltzer, DDS, MScD
Craig Misch, DDS, MDS
Stephan Porter, DDS, MSD, MS
Robert del Castillo, DMD
Ronnie J. Goene, DDS
Abstract:
For years, dental implants have been loaded immediately upon implant placement with varying degrees of success. As clinicians understanding of the biological and mechanical factors involved in immediate occlusal loading (IOL) has evolved, the success of these procedures has increased- particularly as a treatment option for the restoration of the edentulous mandible or the mandible that will be rendered edentulous during treatment. Due to increasing interest in this treatment alternative, the authors have provided a clear definition of the terminology associated with IOL and have demonstrated the DIEM Guidelines used to increase the success and predictability of such treatment. This presentation also introduces new implant components that simplify the clinical application of the immediate loading concept, enhancing its benefits and acceptance among dental patients and practices alike.
The concept of immediately loading dental implants is not novel but extends back to the 1960s, when implant dentistry was still in its relative infancy. While implants of that period were often placed and immediately loaded, they did not always achieve the success rates that are observed and accepted today. Branemark et al subsequently defined a surgical and restorative protocol that significantly increased the predictability of implant-supported prostheses. As a result of this protocol, implant dentistry has gained in popularity and success as a means of treating edentulous patients.
While Branemark listed several requirements for achieving implant success (including no radiographs until second stage surgery, submerged placement, etc.), one of the principal determinants of success was the unloaded healing period postsurgery. According to the original Branemark protocol, dental implants, regardless of their design or system, required and undisturbed healing period of three months in the mandible and six months in the maxilla. While these periods purportedly allowed time for osseointegration of the implants within the respective arch, Branemarks recommendations for healing were based on empirical data that were never scientifically proven and never experimentally ascertained. Branemark granted that his results did not permit statistical evaluation of the separate parameters he believe contributed to the groups success. As implantology has experienced numerous advances in implant designs as well as the surgical and restorative techniques, many clinicians have questioned whether or no the nonloaded healing period is still a valid prerequisite for success. Complicating the issue, however, is that different definitions have been used to describe immediate loading, and it can be difficult for one to arrive at a clear understanding of the involved materials and clinical requisites.
This presentation defines the concepts involved in the immediate loading of dental implants; it also highlights the clinical requisites and components that improve the predictability and ease of use of the DIEM Guidelines. Additionally, it presents the authors consensus regarding the surgical and restorative methods that maintain clinicians expectations with this implant technique.
Definitions of Immediate Loading
The numerous investigators who have explored immediate loading have done so with different definitions and evaluation criteria, which has understandably contributed to the confusion that often surrounds the concept. It has been described as long as a 20-day period, a 30-day period, and is sometimes implied even when the implant restoration is not under full occlusal load. At this time, the authors define the related terms accordingly:
Immediate Occlusal Loading (IOL)- An implant is placed with adequate primary stability; its corresponding restoration ahs full centric occlusion in maximum intercuspation and must be placed with 48 hours postsurgery. This process is based on the design of the restoration to prevent micromotion of the implant.
Immediate Non-occlusal Loading- An implant is placed with adequate primary stability but is not in functional occlusion. These implant restorations are essentially used for aesthetic purposes, frequently in single-tooth or short-span applications. Immediate non-occlusal loading is often performed to provide the patient with aesthetic or psychological benefit during implant therapy, particularly when a provisional removable prosthesis is undesirable during the healing period.
Early Loading- an implant is placed with adequate primary stability and is placed under full occlusal load and prosthetic function within two months. A fundamental goal of early loading is improving bone formation in order to support occlusal loading at two months. Early loading, in contrast to immediate occlusal loading, is based on the interactions of the implant surface with the host bone for achieving biological implant stability.
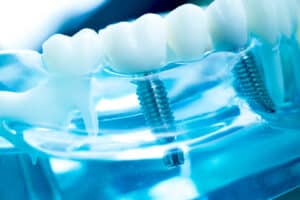
Implant Stability
A fundamental requisite for IOL is adequate primary implant stability. While stability was traditionally achieved through a period of undisturbed healing (i.e., osseointegration), primary stability is now achieved via a mechanical phenomenon of screw stability and splinting. Primary implant stability can be measured via insertion torque values or resonance frequency analysis (RFA). The connection of implants to preexisting rigid members such as stable teeth or integrated implants may also address the goal of preventing lateral movement (i.e., micromotion) of the implant during healing as well.
Each implant system tolerates micromotion differently. For implants with roughened surfaces, tolerance is in the range of 50 to 150 microns, machined surfaces can withstand approximately 100 microns of micromovement. Regardless of the type of implant selected, all restorative procedures should be completed within two days of implant placement according to the specific needs of the patient and after which time bone healing and implant stability may be disrupted by such intervention.
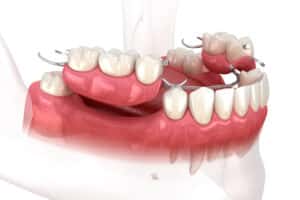
Indications for the Fully Edentulous Mandible
Each patient must be evaluated preoperatively to ensure that he or she satisfies clinical criteria for an IOL protocol, of which requisites include the following:
Adequate bone quality (Types I, II, or III)
Sufficient bone height (i.e., approximately 12mm) for a minimum length 10mm implant
Sufficient bone width (i.e., approximately 6mm)
Ability to achieve an adequate anterior-posterior (AP) spread between the implants. A poor AP spread decreases the mechanical advantage gained by splinting and the ability to cantilever the restoration
Contraindications for the Fully Edentulous Mandible
An immediate loading DIEM protocol is generally contraindicated in patients with the following conditions:
Poor systemic health
Severe parafunctional habits
Bone of poor quality (eg, Type IV bone)
Bone height less than 12 mm
Bone width less than 6mm
Inability to achieve an adequate AP spread.
Advantages and Disadvantages of Immediate Occlusal Loading
The immediate occlusal loading of implants continues to be the subject of clinical investigations due in part to the advantages that it presents to dental professionals. Among these benefits are the following:
Eliminates the need for an maintenance of a removable provisional prosthesis
Provides emotional benefit for a patient scheduled to be rendered edentulous
Improves bone healing
Facilitates soft tissue shaping
Eliminates premature implant exposure often associated with wearing of a removable denture during healing period.
Immediate loading can be advantageous to dental patients as well. In publications regarding conventional implant treatment, patients have cited complaints that include 1) loose-fitting dentures, 2) denture sore spots, 3) difficulty chewing, 4) difficult postoperative periods, and 5) the number of visits required to maintain the prosthesis. Immediate implant loading provides improved function, aesthetics, and psychological benefits to such patients, and it can have a favorable cost/benefit with regard to timing of treatment.
This approach cannot, however, be applied to every implant patient. In comparison to conventional implant therapy, the IOL procedure requires more chair time at the time of implant placement for both the patient and the restorative practitioner. Immediate loading also requires effective communication and coordination among the surgical and restorative teams, as there is a degree of flexibility involved in the delivery of the prosthesis. For example, the surgical and restorative procedures can be completed in a single appointment for straightforward cases. For other cases, the prosthesis may be more appropriately delivered one to two days following implant placement, and the clinician must understand the difference between these options. Careful patient screening and selection are required when an IOL procedure is a treatment consideration. As mentioned previously, immediate loading requires adequate primary stability as well as bone quality.
Investigations and Experiences
Numerous investigators have studied immediate implant loading in order to more full understand the variable that influence its success, yielding more than 50 publications on the topic in 2003 alone. Based on a recent review of 153 publications on immediate loading, Del Fabbro et al have confirmed the effectiveness and safety of its application in the full edentulous mandible.
Other investigations have sought to confirm the efficacy of immediate loading by measuring the extent of osteogenesis and bone remodeling around OSSEOTITE implants (3i, Implant Innovations, Inc., Palm Beach Gardens, FL) placed using this protocol. Clinical and histological examination of two implants retrieved from the 12 implants originally placed in the patient using the IOL procedure revealed high levels of bone-to-implant contact (BIC) that ranged from 78% to 85%. These findings for bone apposition have been achieved in similar studies in which both loading and unloading implants have been placed, allowed to integrate, and were later (after two months) retrieved. Upon examination, all OSSEOTITE implants were clinically stable, and histological examination revealed BIC of 38.9% and 64.2% for unloaded and loaded implants, respectively. Most interestingly, the authors discovered that if an IOL procedure was used and the implants were stabilized throughout the follow-up period, bone apposition would increase around the implant. These results were consistent with those of additional long-term studies on more patients with greater numbers of implants. Each of these IOL procedures was successful to a significant extent based on the clinicians ability to limit micromotion with the provisional prosthesis and to achieve cross-arch stabilization.
These findings have confirmed similar results achieved in animal models. In the histological study preformed by Piatelli et al, BIC immediately occlusally loaded test subjects (67.3% in the maxilla and 73.2% in the mandible) was greater than in non-immediately loaded control subjects (54.5% in the maxilla and 55.8% in the mandible). In the histological and histomorphometric evaluation, immediately loaded and splinted implants in the mandible demonstrated a hard tissue response similar to that of delayed loaded implants. These investigators also included that BIC was the same and that IOL appeared to increase the ossification of the alveolar bone around the implants.
Extrapolating From Clinical Data On Successful Implant Placement
Long-term data evidencing the success rates of the OSSEOTITE implant future supports the IOL of the edentulous mandible. Based on the proven success of the implant survival, prosthesis survival and aesthetics, all of are supported by controlled human multi-center studies; the authors have adopted DIEM Guidelines (from the Latin word for day) and specifically designed IOL Components for the predictable treatment of the fully edentulous mandible or the mandible that will be rendered fully edentulous during treatment.
The armamentarium supporting DIEM is simple to use, inexpensive, and provides the practitioner with flexibility to address a wide variety of clinical conditions during treatment. In this last regard, DIEM can be used with either internally connected or externally hexed parallel wall or tapered implants as well as definitive prostheses of varying styles (e.g., metal-ceramic bridges or fixed detachable bridges). Using this technique and the associated IOL Components, dental professionals can now overcome many of the limitations (e.g., duration of anesthesia, fatigue, patient bleeding, lack of distal prosthesis support) that had traditionally complicated immediate loading procedures. Ultimately, the DIEM Guidelines allow the practitioner to deliver predictable results, ensuring that patient care and the long-term success of the definitive prosthesis remain the focus of the restorative procedure.
Demonstration of the DIEM Guidelines and IOL Components
Treatment planning according to the DIEM Guidelines generally follows the accepted surgical protocol for an IOL procedure. Thus, the appropriate provisional prosthesis and/or surgical guides must be prepared prior to implant placement. When preparing the surgical guide, the guide holes should be positioned so that the implant locations provide an adequate AP spread. Alternately, holes can be drilled in the patients existing denture in the desired implant positions. Once the stability of the denture is verified intraorally, the opposing occlusion must be evaluated. The use of the DIEM Guidelines depends on the patients ability to achieve maximum intercuspation in order to facilitate the construction of the provisional prosthesis. A bite registration is necessary to minimize occlusal adjustments on the provisional prosthesis.
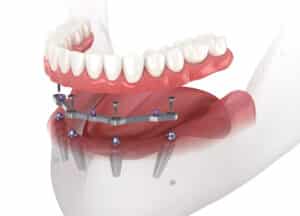
Implant Placement
The ridge of the patients mandible is prepared with the required releasing incisions and flap elevation. The denture or surgical guide is the n placed to facilitate visualization and location of the five implants that will support the provisional prosthesis. Any OSSEOTITE implant can be used with the DIEM procedure and the IOL components. Any adjustments in location or protocol required to ensure a proper AP spread and primary stabilization should also be performed. The classical drilling should then be performed for the operators implant of choice. Site preparation is initiated with a 2mm twist drill. Once this initial drill is withdrawn from the site, a direction indicator pin is placed to allow verification of the denture or surgical guides position. The osteotomy then continues to the proper depth with the corresponding drills. This sequence should first be performed for the most central implant, then for the two most posterior implants, and then the two remaining sites. The implants were placed according to the manufacturers protocol, and forward torque is then applied to at least 20 Ncm to confirm primary stability. If the implants are stable in the mandible, the DIEM procedure can continue; if the implants exhibit some degree of motion, then the clinician should opt instead for a two-stage surgical technique with a non-loaded protocol.
Placement of IOL Abutments
The IOL Abutments are selected and placed with the abutment driver. To facilitate cleansing and function, excess resin and all flanges should be removed, and the denture should be polished prior to intraoral placement. Occlusion is then evaluated, and any undesirable contact areas are eliminated. The denture is then returned to the patients mouth, placed on the abutments, and secured with Gold-Tite retaining screws and 10 Ncm of torque.
The patient should be placed on a soft died for a two-week period and return for evaluation. At approximately eight weeks following the initial implant placement, the immediate fixed provisional restoration can be removed for the first time to permit the impression making required for the fabrication of the definitive prosthesis.
Conclusion
Clinicians search for means of restoring their patients efficiently and effectively is not novel, nor is the concept of immediate implant loading. Reports on IOL procedures continue to proliferate in the literature and, while advocating different protocols, they demonstrate the overall successes on which the DIEM Guidelines are based. The DIEM technique highlighted herein is predicated on the combination of biological and mechanical guidelines, and the adaptation of existing prosthetic concepts, and new data. When supplemented by innovative implant components, these factors provide dental professionals with a set of simple guidelines to produce successful outcomes in a variety of offices with dentists working independently or as part of a team. This approach allows the clinician to customize the technique to the anatomical differences among patients, thus avoiding the need to modify patient treatment to fit a given restorative solution. Future considerations for IOL and other dedicated components and the DIEM Guidelines include their application in the maxilla and partially edentulous patients. While preliminary data collected for these sits are promising, further research and evaluation is ongoing to confirm their long-term success and potential for use in daily restorative practice.